Yes, you can see a General Practitioner (GP) for a skin issue. GPs are often the first point of contact for patients seeking medical advice, and they are trained to manage a wide range of health issues, including skin conditions, whether for yourself or for your child.
Depending on the nature and severity of your skin issue, your GP may be able to diagnose and treat the problem. For example, common skin conditions such as acne, eczema, and psoriasis can often be managed by a GP.
It’s important to note that some GPs may have a special interest in dermatology and have undergone additional training in this area. If you have a specific skin concern, you may wish to ask your GP if they have any particular expertise in this area.
What are 7 common skin problems?
There are many different types of skin problems but here are 7 common ones:
- Acne: Acne is a common skin condition that causes pimples, blackheads, and whiteheads. It can occur anywhere on the body but is most often found on the face, back, and chest.
- Eczema: Eczema is a chronic skin condition that causes red, itchy, and dry skin. It can occur at any age and is often found on the hands, feet, and the creases of the elbows and knees.
- Psoriasis: Psoriasis is a chronic skin condition that causes red, scaly patches on the skin. It can occur anywhere on the body but is often found on the elbows, knees, and scalp.
- Rosacea: Rosacea is a skin condition that causes redness, flushing, and visible blood vessels on the face. It can also cause pimples and thickened skin.
- Hives: Hives are a type of allergic reaction that causes raised, red, and itchy welts on the skin. They can occur anywhere on the body and often appear suddenly.
- Warts: Warts are small, raised growths on the skin caused by a viral infection. They can occur anywhere on the body but are most commonly found on the hands and feet.
- Athlete’s foot: Athlete’s foot is a fungal infection that causes redness, itching, and cracking of the skin on the feet. It is common in athletes and people who wear tight-fitting shoes.
These are generally the most common conditions patients visit a GP for skin problems and can be easily treated with topical treatment or in certain cases, with oral medications. If you are not sure what skin condition you are experiencing, check in with your trusted GP.
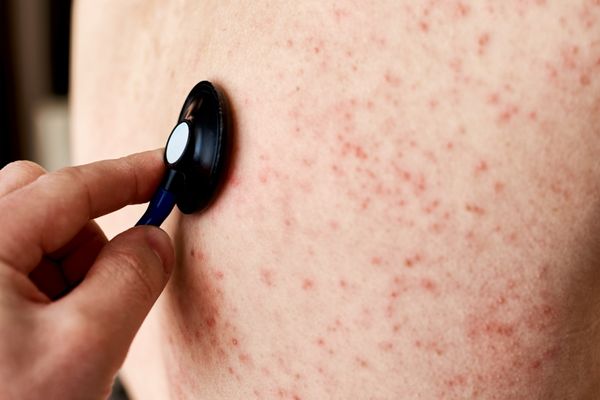
Can I go to the doctors about my skin?
Yes, you can definitely go to the doctor about any concerns you have regarding your skin. Your doctor can help diagnose and treat a variety of skin conditions, ranging from minor issues like acne or rashes to more serious conditions like skin cancer.
In fact, many people see their doctor for skin issues, as a doctor can provide expert advice and treatment for a wide range of skin concerns. Additionally, if your doctor determines that your skin condition requires further evaluation or specialized care, they can refer you to a dermatologist or other specialist for further evaluation.
It’s always a good idea to get any new or concerning skin changes checked by a medical professional. Early detection and treatment of skin conditions can be important for the best outcomes.
How do doctors check your skin?
When a doctor checks your skin, they will typically perform a physical exam and may use various tools or techniques to examine your skin in more detail. In a GP setting, oftentimes, we rely on just visual inspection, by looking out for any visible signs of skin problems, such as rashes, lesions or discolouration.
During the skin exam, the GP may also ask you questions about your medical history, any medications you are taking, and your lifestyle to help determine the cause of your skin problem.
For more complex skin issues that are reviewed by a dermatologist, here are some additional tools they use for diagnosis and treatment of skin issues:
- Dermatoscope: A dermatoscope is a handheld instrument that allows the doctor to examine your skin in more detail. The dermatoscope uses a magnifying lens and a light source to help the doctor see the skin more clearly.
- Wood’s lamp: A Wood’s lamp is a special type of lamp that emits ultraviolet light. The doctor may use this lamp to examine your skin for fungal or bacterial infections, as certain types of infections can appear fluorescent under the Wood’s lamp.
- Biopsy: If the doctor suspects a more serious skin condition, they may take a small sample of skin for further analysis. This is called a skin biopsy and involves removing a small piece of skin tissue for examination under a microscope.
- Patch test: If the doctor suspects you may have an allergic reaction to a substance, they may perform a patch test. This involves placing small amounts of different substances on your skin and monitoring your skin’s reaction to each substance over several days.
How can skin problems be diagnosed?
Skin problems can be diagnosed through a variety of methods, depending on the type and severity of the condition. Here are some common methods that doctors use to diagnose skin problems:
- Physical examination: The doctor will visually inspect the affected skin to look for any signs of rashes, lesions, bumps, or other abnormalities. The doctor may ask questions about the duration of the condition, any symptoms, and any factors that may have triggered the condition.
- Skin biopsy: If the skin condition is severe or the doctor suspects a more serious condition, they may perform a skin biopsy. A skin biopsy involves taking a small sample of skin tissue to examine under a microscope.
- Blood tests: Blood tests may be performed to determine if a skin condition is related to an underlying health condition, such as an autoimmune disorder.
- Allergy testing: If a skin condition is suspected to be related to an allergy, the doctor may perform allergy testing to identify any potential triggers.
- Imaging tests: In some cases, imaging tests such as X-rays, CT scans, or MRI may be used to help diagnose certain skin conditions, such as skin cancer or skin infections.
Once the doctor has made a diagnosis, they can develop a treatment plan tailored to the specific skin condition. Treatment may include medication, topical creams or ointments, lifestyle changes, or other interventions depending on the type and severity of the condition.
What skin disorders are the most serious?
There are several skin disorders that can be serious, depending on the severity of the condition and other factors. These need to be reviewed by a dermatologist and may even require hospital admission for prompt treatment and resolution.
Here are some examples of serious skin disorders:
- Skin cancer: Skin cancer is a potentially life-threatening condition that can develop when skin cells are damaged by the sun’s UV rays. The most serious type of skin cancer is melanoma, which can spread to other parts of the body if not caught and treated early.
- Stevens-Johnson syndrome: Stevens-Johnson syndrome is a rare but serious skin disorder that can cause a severe allergic reaction to medication or infection. It can cause painful blisters and sores on the skin and mucous membranes, as well as other complications.
- Epidermolysis bullosa: Epidermolysis bullosa is a rare genetic disorder that causes the skin to be very fragile and easily damaged. It can lead to painful blisters and sores, as well as other complications.
- Lupus erythematosus: Lupus is an autoimmune disorder that can affect various parts of the body, including the skin. It can cause a butterfly-shaped rash on the face, as well as other skin problems.
- Necrotizing fasciitis: Necrotizing fasciitis is a rare but serious bacterial infection that can affect the skin and other soft tissues. It can cause tissue death and other complications.
It’s important to note that while these skin disorders can be serious, with proper diagnosis and treatment, many people can manage these conditions and lead healthy lives. If you have any concerns about your skin health or are experiencing symptoms of a skin disorder, it’s important to speak with a doctor or dermatologist.
Can stress cause skin problems?
Yes, stress can cause or contribute to certain skin problems. When you are stressed, your body releases hormones such as cortisol, which can affect your skin. Here are some skin problems that can be caused or worsened by stress:
- Acne: Stress can trigger an increase in oil production and inflammation, which can lead to acne breakouts.
- Eczema: Stress can cause or worsen eczema symptoms, such as dry, itchy, and inflamed skin.
- Psoriasis: Stress can trigger psoriasis flare-ups and worsen symptoms such as red, scaly patches on the skin.
- Hives: Stress can cause hives or make existing hives worse.
- Excessive sweating: Stress can trigger excessive sweating, which can lead to skin irritation and other skin problems.
- Rosacea: Stress can trigger rosacea flare-ups and worsen symptoms such as redness, bumps, and skin sensitivity.
It’s important to note that while stress can cause or worsen these skin problems, it is not always the sole cause. Other factors such as genetics, environmental triggers, and other medical conditions can also contribute to skin problems.
If you are experiencing skin problems, it’s always a good idea to speak with a GP to determine the cause and receive appropriate treatment. Additionally, managing stress through relaxation techniques, exercise, and other stress-reduction strategies may help improve skin health.

What causes skin to itch like crazy?
There are many possible causes of itchy skin, some of which can be more serious than others. Here are some common causes of itchy skin:
- Dry skin: When skin becomes too dry, it can become itchy and flaky. This is a common problem in the winter or in dry climates.
- Allergic reactions: Allergies to certain foods, medications, or other substances can cause itchy skin.
- Insect bites: Mosquitoes, fleas, and other insects can cause itchy skin when they bite.
- Skin infections: Certain skin infections such as ringworm, scabies, or a yeast infection can cause itchy skin.
- Eczema: Eczema is a chronic skin condition that can cause itchy, inflamed, and scaly skin.
- Psoriasis: Psoriasis is a chronic autoimmune disorder that causes itchy, scaly patches on the skin.
- Hives: Hives are itchy, raised welts that can be caused by an allergic reaction to food, medication, or other substances.
- Contact dermatitis: This is a type of skin rash caused by an allergic reaction to a substance that comes into contact with the skin, such as poison ivy or certain chemicals.
- Stress and anxiety: Stress and anxiety can cause or worsen itchy skin.
If you have itchy skin that is accompanied by other symptoms such as a rash, redness, or swelling, or if the itching is severe or persistent, it’s important to speak with a GP to determine the cause and receive appropriate treatment.
Why am I itchy all over at night?
Itchy skin at night can be caused by a variety of factors. Here are some possible reasons why you might be experiencing nighttime itching:
- Dry skin: Skin tends to lose moisture at night, which can make it feel dry and itchy. This can be worsened if the air in your bedroom is dry.
- Bedbugs: Bedbugs can cause itchy red bites that often appear in clusters on the skin. They are usually found in or near the bed, and can be difficult to get rid of.
- Allergies: Allergies to dust mites, pet dander, or other allergens in your bedroom can cause itchy skin at night.
- Skin conditions: Skin conditions such as eczema, psoriasis, or hives can cause itchy skin at night.
- Stress and anxiety: Stress and anxiety can cause or worsen itching, and may be more noticeable at night when you are trying to relax.
You can try taking a cool bath or shower before bed, using a moisturizing lotion, wearing loose clothing to bed, and using a humidifier in your bedroom to help relieve dry skin and itching. If the symptoms are persistent, go visit your trusted GP to find out if they could be a sign of something more serious.
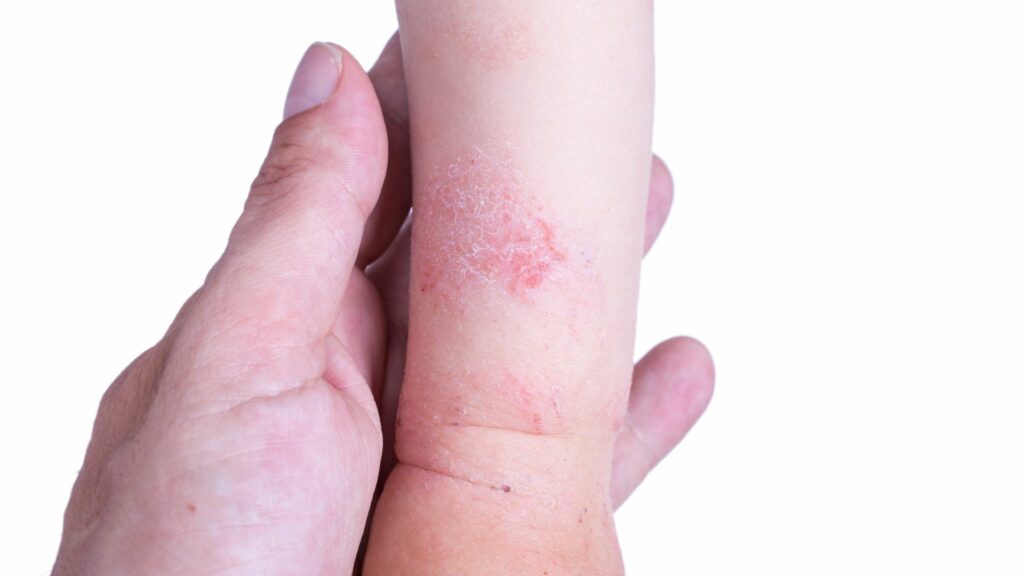
Can stress cause itchy skin?
Yes, stress can cause itchy skin. When you are stressed, your body releases a hormone called cortisol, which can affect your immune system and cause inflammation. Inflammation can trigger itching, redness, and other skin reactions.
Stress can also worsen existing skin conditions, such as eczema, psoriasis, and hives. Additionally, stress can cause you to scratch your skin more often or more intensely, which can worsen itching and cause further damage to your skin.
If you are experiencing itchy skin due to stress, there are several things you can do to help manage the symptoms. These may include stress-reducing activities such as exercise, yoga, or meditation, as well as getting enough sleep and eating a healthy diet.
You can also speak with your GP to discuss treatment options for any underlying skin conditions that may be causing the itching. They may recommend topical creams or medications to help relieve symptoms.
What deficiency causes skin itching?
A deficiency in certain vitamins and minerals can cause skin itching. Here are some deficiencies that can cause this symptom:
- Vitamin D: Vitamin D deficiency is a common cause of itchy skin. Vitamin D is important for healthy skin, and a deficiency can cause dryness and itching.
- Vitamin B12: Vitamin B12 deficiency can cause a variety of skin symptoms, including itching, dryness, and rashes.
- Iron: Iron deficiency can lead to dry, itchy skin, and in severe cases, can cause a condition called restless leg syndrome, which can cause itching and discomfort.
- Zinc: Zinc is essential for healthy skin, and a deficiency can cause skin problems including itching and rashes.
If you suspect that a vitamin or mineral deficiency may be causing your skin itching, it’s important to speak with a doctor to get a proper diagnosis and treatment. Blood tests can easily be done with your GP to detect Vitamin D, Vitamin B12 or Iron deficiency and they can be treated with diet changes or supplements.
It’s also important to note that many other conditions and factors can cause skin itching, so it’s important to get a proper diagnosis to determine the underlying cause.
Can itchy skin be caused by kidney problems?
Yes, itchy skin can be a symptom of kidney problems. When the kidneys are not functioning properly, they may not be able to filter waste products and excess fluid from the body effectively. This can lead to a buildup of waste products in the bloodstream, which can cause itching and other skin symptoms.
In particular, kidney disease can lead to a buildup of uremic toxins in the body, which can cause itching. Itching is more common in advanced stages of kidney disease, and may be more severe in people who are on dialysis.
If you have itchy skin and suspect that it may be related to your kidneys, it’s important to speak with a doctor. They can perform tests to check your kidney function and determine the underlying cause of your symptoms. Treatment for kidney-related itching may involve managing the underlying kidney condition, taking medications to relieve itching, and making lifestyle changes such as avoiding irritants that may make itching worse.
Is itchy skin a symptom of anything serious?
Itchy skin can be a symptom of many different conditions, ranging from mild to serious. In some cases, itchy skin may be a sign of a more serious underlying health condition. Here are some examples:
- Kidney disease: Itchy skin can be a symptom of kidney disease or kidney failure. When the kidneys are not functioning properly, waste products can build up in the blood and cause itching.
- Liver disease: Itchy skin can also be a symptom of liver disease, such as cirrhosis or hepatitis. Liver disease can cause bile to build up in the blood, which can lead to itching.
- Thyroid problems: An overactive or underactive thyroid can cause itching and other skin symptoms.
- Cancer: Itching can be a symptom of certain types of cancer, such as lymphoma.
- Autoimmune diseases: Autoimmune diseases, such as lupus or celiac disease, can cause itchy skin.
- Medications: Itching can be a side effect of certain medications, such as opioids, antibiotics, or chemotherapy drugs.
If you are experiencing persistent or severe itching, it’s important to speak with a doctor to determine the underlying cause and receive appropriate treatment. They may perform tests or refer you to a specialist to help diagnose the condition. While many cases of itchy skin are not serious, it’s important to rule out any underlying health problems that may require medical attention.
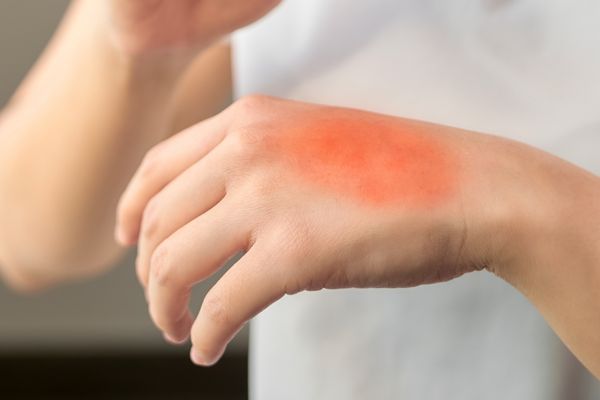
When should I be worried about itchy skin?
You should be worried about itchy skin if it is persistent, severe, or accompanied by other symptoms. Itching is a common symptom of many conditions, ranging from mild to serious. In most cases, itchy skin is not a cause for concern and can be treated with over-the-counter remedies or lifestyle changes.
However, here are some situations in which you should seek medical attention for your itchy skin:
- If the itching is severe and affecting your quality of life.
- If the itching is accompanied by other symptoms such as rash, hives, or swelling.
- If the itching is all over your body and does not go away with home remedies.
- If the itching is persistent and lasts for more than two weeks.
- If the itching is spreading rapidly or getting worse.
- If the itching is associated with any other concerning symptoms, such as weight loss, fatigue, or fever.
- If you have a known medical condition that may be causing the itching, such as kidney disease or liver disease.
If you are experiencing any of these symptoms, it’s important to speak with a GP to determine the underlying cause and receive appropriate treatment. They may be able to administer some simple forms of treatment and monitor your response accordingly. In addition, they may perform tests or decide to refer you to a specialist if the diagnosis is dangerous or you are not responding to common remedies.
Should I tell my doctor about my acne?
Yes, it’s a good idea to tell your doctor about your acne. Acne is a common skin condition that affects many people, and it can have a significant impact on your quality of life. While mild acne can often be managed with over-the-counter products, more severe or persistent acne may require medical treatment.
Your doctor can help you determine the underlying cause of your acne and develop a treatment plan that is tailored to your specific needs. They can also prescribe medications or topical treatments that are more effective than over-the-counter remedies.
In addition, your doctor can help you identify any factors that may be contributing to your acne, such as hormonal imbalances, diet, or stress. By addressing these underlying issues, you may be able to improve your skin health and reduce your risk of future breakouts.
Overall, it’s important to be open and honest with your doctor about any skin concerns you may have, including acne. They can provide you with the guidance and support you need to manage your condition and achieve clearer, healthier skin.
Can a GP diagnose acne?
Yes, a GP (general practitioner) can diagnose acne. Acne is a common skin condition that can be diagnosed through a physical exam and a discussion of your medical history and symptoms.
During a physical exam, your GP will likely examine your skin to determine the severity and distribution of your acne. They may also ask you about your diet, skincare routine, and any medications or supplements you are taking.
Can a GP help with pimples?
Yes, a GP (general practitioner) can help with pimples. Pimples are a common type of acne, and GPs are trained to diagnose and treat a variety of skin conditions, including acne.
Your GP can examine your skin, ask you about your medical history and lifestyle habits, and recommend a treatment plan based on the severity and type of your acne. Treatment options for pimples may include over-the-counter topical medications, prescription medications, lifestyle changes, or a combination of these.

What acne treatment can the GP prescribe?
A GP (general practitioner) can prescribe a variety of treatments for acne, depending on the severity and type of acne, as well as the patient’s individual needs and preferences. Some common acne treatments that a GP may prescribe include:
- Topical retinoids: These are medications that are applied directly to the skin to unclog pores and reduce inflammation. They work by increasing cell turnover and promoting the growth of new skin cells.
- Topical antibiotics: These are medications that are applied directly to the skin to kill bacteria and reduce inflammation. They can be particularly effective for inflammatory acne.
- Oral antibiotics: These are medications that are taken orally to kill bacteria and reduce inflammation. They can be particularly effective for moderate to severe acne.
- Oral contraceptives: These are medications that are taken orally to regulate hormones and reduce acne. They can be particularly effective for women with hormonal acne.
- Isotretinoin: This is a powerful medication that is used to treat severe acne that has not responded to other treatments. It works by reducing oil production and unclogging pores. However, isotretinoin can have serious side effects, so it is only prescribed under close medical supervision.
Overall, the treatment approach for acne will depend on the type and severity of the acne, as well as the patient’s individual needs and preferences. It’s important to consult with a GP to determine the most appropriate treatment plan for your specific case.
Can GPs prescribe antibiotics for acne?
Yes, GPs (general practitioners) can prescribe antibiotics for acne. Antibiotics are often used to treat inflammatory acne, which is characterized by redness, swelling, and pus-filled bumps. Antibiotics work by killing the bacteria that contribute to acne, reducing inflammation, and preventing the formation of new pimples.
There are both topical and oral antibiotics available for acne treatment. Topical antibiotics are applied directly to the skin, while oral antibiotics are taken by mouth.
It’s important to note that while antibiotics can be effective in treating acne, they can also have side effects and contribute to antibiotic resistance. As a result, doctors typically only prescribe antibiotics for acne when other treatments have failed, and they may use them in combination with other medications or therapies to optimize results. It’s important to discuss the potential benefits and risks of antibiotic treatment with your GP and to follow their instructions carefully.
Can GPs prescribe Accutane?
Yes, GPs (general practitioners) can prescribe Accutane (isotretinoin) in some countries, although the rules and regulations surrounding its use can vary by location. In Singapore, you are able to get isotretinoin treatment with certain GPs at low doses and with close medical supervision.
Accutane is a powerful medication used to treat severe acne that has not responded to other treatments. It works by reducing oil production and unclogging pores, and is often considered a last resort for treating acne.
However, Accutane can have serious side effects, including birth defects, depression or mood changes, liver damage and elevation of your cholesterol. For this reason, doctors typically only prescribe Accutane under close medical supervision, and patients may need to undergo regular blood tests and other monitoring while taking the medication.
In many cases, patients are required to sign a consent form indicating that they understand the risks and agree to use effective birth control (for women) while taking the medication.
Can GPs prescribe Retinol?
Yes, GPs (general practitioners) can prescribe retinol, which is a type of vitamin A derivative that is commonly used in skincare products to improve skin texture, reduce the appearance of fine lines and wrinkles, and treat acne. Retinol can be prescribed as a cream or gel, and is typically used topically to treat skin concerns.
Retinol is available in different strengths, and it’s important to use it as directed by your GP or healthcare provider to avoid potential side effects, such as redness, irritation, and flaking. Retinol can also make your skin more sensitive to the sun, so it’s important to use sun protection when using this medication.
Should I go to the GP or dermatologist for acne?
If you have mild to moderate acne, you can usually start by visiting your GP (general practitioner) for treatment. GPs are trained to diagnose and treat a wide range of medical conditions, including acne, and can provide you with initial guidance and treatment options. Your GP can prescribe topical or oral medications, recommend lifestyle changes or over-the-counter products, or refer you to a dermatologist for further evaluation if necessary.
If you have severe or persistent acne that does not respond to initial treatment or is causing scarring or other skin damage, your GP may refer you to a dermatologist for specialized care. Dermatologists are medical specialists who focus on the diagnosis, treatment, and prevention of skin conditions, including acne. They can provide a more comprehensive evaluation of your skin, prescribe stronger medications or other treatments, and offer guidance on how to manage your acne over the long term.
Ultimately, whether you should see a GP or a dermatologist for your acne depends on the severity and complexity of your condition, as well as your personal preference. It’s important to discuss your concerns with your GP or healthcare provider, who can help guide you to the appropriate care and treatment for your individual needs.
What does a cancerous rash look like?
A cancerous rash can appear different depending on the type of cancer, but in general, it may have some of the following characteristics:
- Irregular shape: The rash may have an irregular shape or borders, rather than a symmetrical or round shape.
- Abnormal color: The rash may appear to be a different color than the surrounding skin, including shades of red, brown, or black.
- Increased size: The rash may grow or spread over time, becoming larger or developing additional bumps or lesions.
- Itching or pain: The rash may be itchy or painful, which can be a sign that it is cancerous.
- Bleeding or crusting: The rash may bleed or develop a crust, which can indicate that the cancerous cells are breaking down the skin’s tissue.
It’s important to note that not all rashes are cancerous, and there are many non-cancerous causes of skin rashes. If you have a rash that concerns you, it’s important to see a healthcare provider for an evaluation and diagnosis. They can help determine the cause of your rash and recommend appropriate treatment.
Is itchy skin cancerous?
Itchy skin is not necessarily a sign of skin cancer. Many different conditions which are much more commonly seen, can cause itchy skin, including dry skin, eczema, allergies, insect bites, and certain medications. However, itchy skin can sometimes be a symptom of certain types of skin cancer, such as basal cell carcinoma or cutaneous T-cell lymphoma.
In general, if you have itchy skin that does not go away or worsens over time, it’s important to see a healthcare provider for an evaluation. They can help determine the underlying cause of your itching and recommend appropriate treatment if necessary. If they suspect that your itching is related to skin cancer, they may recommend further testing or refer you to a specialist for further evaluation and treatment.
What cancers cause itching skin?
Several types of cancer can cause itching skin, including:
- Hodgkin’s lymphoma: This type of cancer affects the lymphatic system and can cause itchy skin, especially after exposure to hot water.
- Non-Hodgkin’s lymphoma: Like Hodgkin’s lymphoma, non-Hodgkin’s lymphoma affects the lymphatic system and can cause itching skin.
- Cutaneous T-cell lymphoma: This rare type of lymphoma affects the skin and can cause itchy patches or plaques.
- Leukemia: This type of cancer affects the blood and bone marrow and can sometimes cause itchy skin.
- Liver cancer: When cancer cells invade the liver, they can cause a buildup of bile salts in the blood, leading to itchy skin.
- Pancreatic cancer: In rare cases, pancreatic cancer can cause itchy skin as a result of the buildup of certain substances in the blood.
It’s important to note that not all cases of itching skin are caused by cancer and the above cancers are rare. If you have persistent or unexplained itching that does not respond to treatment for common skin conditions, it is important to see a healthcare provider for an evaluation to determine the underlying cause and receive appropriate treatment.
Can a GP tell if a spot is cancerous?
A GP can sometimes tell if a spot or skin lesion is cancerous, but they may also refer you to a dermatologist or specialist for further evaluation and testing.
During a skin exam, a GP will usually look at any spots or lesions on your skin and may ask about your personal and family medical history.
However, skin cancer can be difficult to diagnose based on appearance alone, as many non-cancerous spots can look similar to cancerous ones. Therefore, if you have any spots or lesions that are changing, growing, or bleeding, or if you are concerned about a spot on your skin, it’s important to seek medical attention as soon as possible for an accurate diagnosis and appropriate treatment.
What doctor should I see for skin problems?
Who should you consult for any skin concerns?
For most routine skin concerns, you can start by consulting a primary care physician or general practitioner (GP). They are trained to diagnose and treat common skin conditions, such as acne, eczema, psoriasis, and rashes. Depending on the nature and severity of your skin concern, they may prescribe topical or oral medications, recommend lifestyle changes or over-the-counter products.
If your skin concern is more complex or severe, or if you have a history of skin cancer or other serious skin conditions, you may want to see a dermatologist, who is a medical specialist trained to diagnose and treat conditions of the skin, hair, and nails.
In general, it’s a good idea to consult with a healthcare professional if you have any concerns about your skin. They can help you understand your symptoms, diagnose any underlying conditions, and recommend appropriate treatment options to help you manage your skin health.
Can a GP help with skin problems?
Yes, a GP (general practitioner) can help with many types of skin problems. GPs are trained to diagnose and treat a wide range of medical conditions, including skin issues such as acne, rashes, eczema, psoriasis, and infections.
When you visit a GP for a skin problem, they will typically examine the affected area and ask you questions about your symptoms, medical history, and lifestyle. Depending on their evaluation, they may prescribe topical or oral medications, recommend over-the-counter products or lifestyle changes.
In some cases, your GP may also perform minor procedures such as removing a mole, cyst, or skin tag, or taking a sample of skin for further testing. However, for more complex or severe skin problems, your GP may refer you to a dermatologist or other specialist for further evaluation or treatment.
Overall, GPs can provide important guidance and treatment options for many types of skin problems, and can also help coordinate your care with other healthcare providers as needed.
Can I go to a polyclinic for skin issues?
Yes, you can usually visit a polyclinic for skin issues. Polyclinics are medical facilities that provide a wide range of general medical services, including primary care services, to patients in a community setting. Many polyclinics have doctors who are trained to diagnose and treat common skin conditions, such as acne, eczema, psoriasis, and rashes. They are also equipped to treat skin problems with topical creams or oral medications as needed.

Can a blood test detect skin conditions?
Some blood tests can help diagnose or monitor certain skin conditions, but not all skin conditions can be detected through blood tests alone. The specific tests recommended will depend on the nature and suspected cause of the skin condition.
For example, blood tests may be useful in diagnosing autoimmune skin diseases, such as lupus, which can cause skin inflammation and damage. In addition, blood tests can sometimes help diagnose skin infections, such as bacterial or viral infections.
However, most skin conditions are not detected through blood tests, and a diagnosis often requires a combination of clinical examination and medical history taken from the patient. In some cases, a skin biopsy may be recommended to determine if a long standing skin issue is something more dangerous.
When should you see a dermatologist?
You should consider seeing a dermatologist for any concerns related to your skin, hair, or nails, especially if you notice any changes or abnormalities. Here are some specific situations where you may want to consider seeing a dermatologist:
- Skin rashes or spots that don’t go away: If you have a rash or spot on your skin that has persisted for more than a few weeks, or that is changing in shape, size, or color, you should see a dermatologist.
- Suspicious moles or other skin growths: If you have a mole or other skin growth that is asymmetrical, has irregular borders, is changing in color, or is larger than 6mm in diameter, you should see a dermatologist.
- Severe acne that is not controlled with low doses of isotretinoin or causing severe scarring.
- Persistent itching or drying that does not respond to common treatment administered by your GP.
These are just a few examples of situations where you may want to consider seeing a dermatologist. It’s important to remember that your skin is your body’s largest organ, and taking care of it is an important part of overall health and wellbeing.
How do I ask for a dermatologist referral?
If you are experiencing a skin condition and would like to see a dermatologist, you can ask your primary care physician or general practitioner (GP) for a referral. Here are some tips on how to ask for a referral:
- Be specific about your concerns: When you speak with your primary care physician or GP, be clear about your skin concerns, and why you think you need to see a dermatologist. If you’ve tried over-the-counter treatments without success, or if you have a family history of skin cancer, for example, be sure to mention these details.
- Request a referral: After you have explained your concerns, you can ask your GP for a referral to a dermatologist.
- Check your insurance coverage: Some insurance plans may require a referral from your primary care physician or GP before you book an appointment with them.
- Follow up: If your primary care physician or GP agrees to give you a referral, be sure to follow up with the dermatologist’s office as soon as possible to schedule an appointment. Be sure to bring any relevant medical records or test results with you to your appointment.
If you have concerns about your skin, don’t be afraid to speak up and ask for a referral to a dermatologist.
What happens when you are referred by your GP to see a specialist?
When you are referred by your GP to see a specialist, the specialist will review your medical history and any relevant test results, and will perform a physical examination to determine the cause of your symptoms. They will also want to know what treatment the GP has already administered and does not work in clearing the skin condition.
The specialist will then work with you to develop a treatment plan, which may include medications, lifestyle changes, or additional testing or procedures. The specialist will communicate with your GP to keep them updated on your progress and any changes to your treatment plan.
In some cases, the specialist may determine that you do not need any further treatment or that your condition can be managed by your GP. In other cases, the specialist may recommend ongoing care or follow-up visits.
It’s important to remember that a specialist referral does not necessarily mean that you have a serious medical condition. Referrals are often made for routine or preventative care, or to ensure that you receive the most appropriate care for your specific needs. If you have any concerns or questions about your referral, your GP can help provide more information.

Conclusion of a Skin Check-up
We have covered the basics of what is involved in diagnosing common skin conditions in a primary care setting and that includes skin issues like eczema and acne. These are generally the most common conditions patients visit a GP for skin problems and can be easily treated with topical treatment or in certain cases, with oral medications. If you are not sure what skin condition you are experiencing, check in with your trusted GP.

GET IN TOUCH
Schedule a Visit

Dr Zhang Huipei
Medical Director
MBBS (Singapore)
Graduate Diploma in Family Medicine
Family Physician
Dr Zhang is in Clinic on Monday, Tuesday, Wednesday, Thursday and Saturday.

Enjoyed looking at this, very good stuff, thanks.